Why Mental Health Billing in San Diego Has Become More Complex Than Most Practices Expect
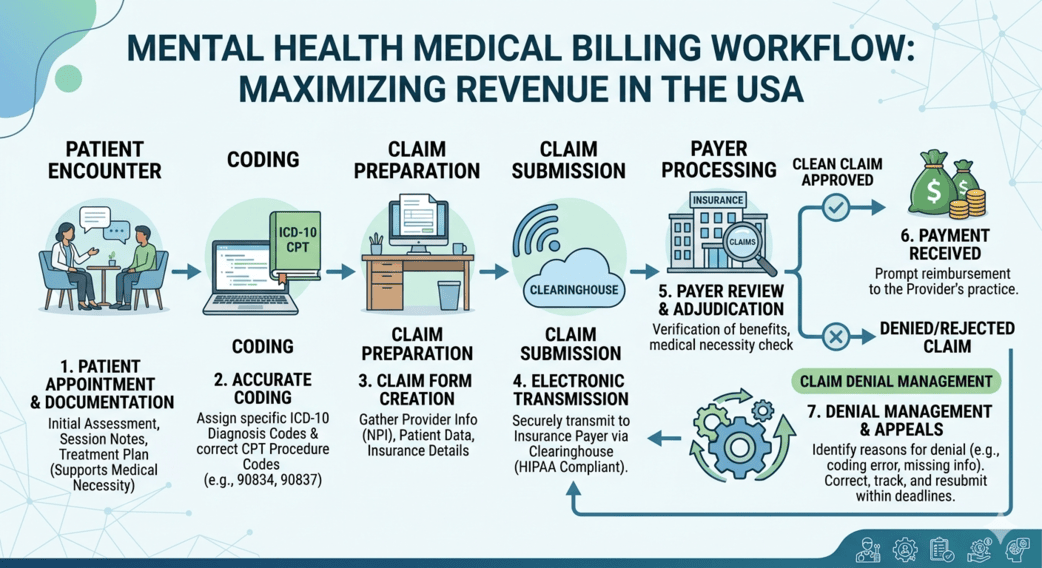
Mental health providers in San Diego are seeing something many clinics across the country are struggling with: patient demand is growing rapidly, but reimbursement is not getting any easier.
Therapists, psychologists, psychiatrists, and behavioral health groups are managing larger caseloads while also dealing with changing payer rules, telehealth regulations, prior authorization requirements, and documentation scrutiny. Even experienced providers often discover that getting paid accurately and on time requires far more administrative work than anticipated.
That’s one reason why mental health billing in San Diego has evolved into a specialized operational function rather than a simple back-office task.
For many practices, the biggest challenge is not attracting patients. It’s maintaining a healthy revenue cycle while continuing to provide quality care without administrative burnout.
The Financial Side of Behavioral Health Is Uniquely Challenging
Mental health billing operates differently from many other medical specialties. Sessions are time-based, coding requirements are nuanced, and insurance carriers frequently apply behavioral health policies that differ from standard medical claims.
A therapist may provide excellent care and complete proper clinical documentation, yet still experience delayed payments because a payer requires additional modifiers, updated treatment plans, or stricter authorization tracking.
In San Diego specifically, providers often work with a mix of:
- Commercial insurance plans
- Medicaid programs
- Employee assistance programs (EAPs)
- Telehealth claims
- Out-of-network reimbursements
- Integrated behavioral health services
Each payer comes with different billing expectations.
This complexity is why many clinics now rely on billing services for mental health therapists that understand behavioral health coding beyond the basics.
Common Revenue Problems Mental Health Practices Face
Many providers assume denials happen mainly because of coding mistakes. In reality, the issues are usually broader and more operational.
Incomplete Documentation Alignment
Behavioral health claims are closely tied to clinical notes and treatment plans. If documentation does not fully support medical necessity, insurers may reject or downcode claims.
For example, a therapist may document anxiety symptoms thoroughly but fail to connect treatment progress to the care plan. That gap can trigger payer scrutiny during audits.
Authorization Tracking Failures
Mental health services often require recurring authorization approvals. Missing even one renewal date can lead to multiple denied sessions.
Small practices handling billing internally frequently struggle with authorization monitoring because front-desk teams are already overloaded with scheduling and patient communication.
Telehealth Billing Confusion
Teletherapy expanded significantly after the pandemic, but payer policies continue to change. Place-of-service codes, modifiers, and reimbursement rules vary widely.
A clinic that bills telehealth incorrectly for just a few months can lose substantial revenue without realizing it immediately.
Delayed Claim Submission
Mental health providers sometimes prioritize patient care so heavily that billing becomes secondary. Unfortunately, delayed submissions can create cash flow instability.
Claims that sit unprocessed for weeks can eventually miss timely filing limits altogether.
Why Outsourcing Is Becoming More Common in Behavioral Health
Several years ago, outsourcing billing was mainly associated with large medical organizations. Today, even solo therapists are considering external billing support.
The reason is simple: administrative pressure is increasing faster than most practices can scale internally.
Outsourced mental health billing allows providers to focus on patient care while specialists handle claim management, coding reviews, payment posting, and denial resolution.
More importantly, experienced behavioral health billers understand the nuances that general medical billers may miss.
A dedicated mental health billing agency often recognizes trends quickly, such as:
- Which payers frequently deny psychotherapy add-on codes
- Which insurers request recurring documentation updates
- Which authorization workflows create delays
- Which coding combinations increase reimbursement risk
That level of specialization matters.
A Small Coding Error Can Create Larger Financial Consequences
Consider a mid-sized counseling practice in San Diego that offers individual therapy, family counseling, and medication management.
The practice notices reimbursements dropping despite stable patient volume.
After reviewing claims, a mental health billing consultant identifies several issues:
- Incorrect modifier usage for telehealth sessions
- Missed opportunities for reimbursable collaborative care services
- Claims submitted under outdated payer requirements
- Inconsistent diagnosis coding across providers
None of these errors seemed catastrophic individually. Together, however, they reduced monthly collections significantly.
After correcting workflows and implementing stronger coding oversight, the clinic improved claim acceptance rates within a few billing cycles.
This scenario is common throughout behavioral health.
Choosing the Right Mental Health Billing Support Matters
Not all billing vendors are equally prepared for behavioral health.
Some general medical billing companies handle multiple specialties but lack deep understanding of psychotherapy workflows, psychiatric coding, or behavioral health payer policies.
That distinction becomes critical when practices scale.
A reliable mental health billing and coding company should understand:
Behavioral Health CPT Coding
Psychotherapy codes require precision, especially when sessions vary by duration or involve add-on services.
Incorrect coding can lead to underpayments or compliance concerns.
Insurance Verification for Mental Health Benefits
Behavioral health coverage limitations are often more restrictive than medical benefits.
Verification teams must confirm:
- Session limits
- Authorization requirements
- Deductibles
- Copays
- Telehealth eligibility
- Out-of-network policies
Denial Management Strategies
Strong denial management goes beyond resubmitting claims.
Experienced mental health billing companies identify recurring denial patterns and improve workflows to prevent future losses.
Compliance and Documentation Support
Behavioral health audits are becoming more frequent. Practices need billing teams that align claims with payer documentation expectations.
The Growing Role of Technology in Behavioral Health Billing
Modern mental health billing is no longer just manual claim entry.
Advanced billing teams now use analytics and automation tools to monitor:
- Aging accounts receivable
- Authorization timelines
- Claim rejection trends
- Provider productivity
- Reimbursement patterns
For example, a behavioral health clinic may notice that one insurance carrier consistently delays reimbursement for certain CPT combinations.
A proactive billing team can flag the issue early and adjust workflows before revenue disruption escalates.
Technology also improves transparency. Many providers now expect real-time reporting instead of waiting until month-end to understand financial performance.
What San Diego Providers Should Look For in a Billing Partner
Mental health practices in San Diego operate in a competitive healthcare environment. Patients expect accessibility, fast scheduling, and flexible care options.
Providers therefore need operational stability behind the scenes.
When evaluating billing services for mental health providers, practices should look beyond basic pricing.
Important considerations include:
Specialty Experience
A vendor experienced in behavioral health understands psychiatric evaluations, therapy coding, medication management billing, and payer-specific mental health policies.
Communication Structure
Practices should know who manages their account and how issues are escalated.
Strong communication reduces confusion and accelerates claim resolution.
Reporting Transparency
Financial reporting should provide actionable insights, not just spreadsheets full of numbers.
Providers need visibility into:
- Collection trends
- Denial categories
- Payer performance
- Outstanding claims
- Authorization bottlenecks
Scalability
A solo therapist today may become a multi-provider practice tomorrow.
The best outsource mental health billing and coding company should support long-term growth without disrupting operations.
Why In-House Billing Often Reaches a Breaking Point
Many providers initially prefer keeping billing internal because it feels more controllable.
But over time, several problems tend to emerge:
- Staff turnover
- Training gaps
- Burnout
- Coding inconsistencies
- Delayed follow-ups
- Limited payer knowledge
Behavioral health billing requires ongoing education because payer requirements continually evolve.
A front-office employee managing phones, scheduling, and claims simultaneously may struggle to maintain billing accuracy consistently.
This is why mental health medical billing services outsourcing has become increasingly common among growing practices.
Outsourcing doesn’t necessarily remove control. In many cases, it improves operational visibility while reducing administrative strain.
The Impact of Denials on Mental Health Practices
Denied claims affect more than revenue.
They can also:
- Disrupt payroll planning
- Delay expansion efforts
- Increase provider stress
- Create patient billing confusion
- Reduce operational predictability
Mental health providers already work in emotionally demanding environments. Constant reimbursement uncertainty only adds pressure.
An experienced top outsource mental health billing company focuses not only on claim submission but also on financial stability.
That includes:
- Faster payment cycles
- Cleaner claims
- Better eligibility verification
- Timely appeals
- Consistent follow-up processes
These operational improvements directly affect practice sustainability.
Outsourcing Does Not Mean Losing the Human Element
Some providers hesitate to outsource because they fear patients will receive impersonal financial communication.
In reality, strong outsourced teams often improve patient experience.
When billing workflows are organized:
- Patients receive clearer statements
- Eligibility issues are identified earlier
- Payment confusion decreases
- Front-desk staff can focus on patient interaction instead of chasing claims
For mental health settings especially, reducing administrative frustration matters.
Patients dealing with anxiety, depression, trauma, or psychiatric conditions benefit from smoother administrative experiences.
Frequently Asked Questions
Why is mental health billing different from general medical billing?
Behavioral health claims involve time-based therapy codes, detailed documentation requirements, authorization tracking, and unique payer policies. These complexities require specialized billing knowledge.
Can small therapy practices benefit from outsourced billing?
Yes. Even solo therapists often struggle with insurance verification, claim follow-up, and denial management. Outsourced mental health billing can reduce administrative workload and improve reimbursement consistency.
What should providers expect from a mental health billing consultant?
A consultant should analyze workflow inefficiencies, coding accuracy, denial trends, payer issues, and revenue cycle gaps while recommending practical improvements.
How do mental health billing companies improve collections?
Specialized billing teams typically improve claim accuracy, reduce denials, track authorizations more effectively, and follow up on unpaid claims faster than overloaded in-house teams.
Is outsourcing secure for behavioral health practices?
Reputable billing partners use HIPAA-compliant systems, secure data handling protocols, and protected communication channels to maintain patient confidentiality.
What services are typically included in behavioral health billing support?
Most providers receive insurance verification, coding assistance, claim submission, payment posting, denial management, reporting, and accounts receivable follow-up.
Looking Ahead: Financial Stability Will Depend on Operational Expertise
Behavioral health demand in San Diego continues to grow, but financial success requires more than clinical excellence alone.
Providers need operational systems capable of handling increasingly complicated payer requirements, coding expectations, and reimbursement rules. Practices that fail to modernize billing workflows often experience rising denials, delayed payments, and administrative exhaustion.
That’s why many organizations are now treating mental health billing in San Diego as a strategic component of practice management rather than a routine administrative task.
Experienced partners can help behavioral health providers strengthen collections, improve workflow efficiency, and reduce compliance risks without disrupting patient care. Companies like 247 Medical Billing Services support practices through specialized medical billing services, medical coding services, and integrated medical billing and coding services designed for evolving healthcare environments.
As behavioral health practices grow, broader operational support also becomes essential. Efficient revenue cycle management, accurate payer coordination, and streamlined credentialing services all contribute to long-term financial stability and sustainable patient care delivery.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Games
- Gardening
- Health
- Home
- Literature
- Music
- Networking
- Other
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness